Sleep Apnea vs. Insomnia: The Differences, Similarities, and Connections
Research shows that 1 in every 15 adults has obstructive sleep apnea. That equates to nearly 18 million Americans. The more alarming statistic is that 80% of patients with this condition go undiagnosed. While the snoring and erratic breathing associated with sleep apnea can be a nuisance, the condition itself is life-threatening, making a quick and accurate diagnosis a must.

Unsure what sleep apnea is or how it can interfere with not only achieving a quality night’s sleep but also your overall health and wellbeing? You’ve come to the right place. Here we’ll explore all there is to know about obstructive sleep apnea (including symptoms, warning signs, causes, and treatment), as well as the impact it has on sleep patterns and its connection to insomnia.
Content
What is Sleep Apnea?
Before we can discuss the connection between insomnia and sleep apnea, we need a better understanding of the condition and its causes.

Obstructive sleep apnea is a serious sleeping disorder that causes sufferers to stop and start breathing numerous times throughout the night. There are 3 types of sleep apnea: obstructive, central, and complex.
Obstructive Sleep Apnea
This type of sleep apnea is the most common and is caused when the muscles in the back of your throat relax too much. The muscles in your throat are designed to support your soft palate, uvula, tonsils, tongue, and side walls of your throat. When these muscles relax, they narrow your airway, creating an obstruction. Oxygen can’t flow freely through your mouth, nose, throat, and into your lungs. At this point, your brain and body sense that you’re in distress and wake you momentarily so you can reopen your airway (gasp for air).
For many people, this moment is so brief that they generally don’t remember it. Others around them might notice long periods of paused breathing followed by gasping or a deep inhale. Other reactions include choking or snorting. These interrupted sleep patterns can happen from 5 to over 30 times per hour throughout the entire night. As you can imagine, this prevents sleep apnea sufferers from achieving deep or restful sleep.
Central Sleep Apnea
Central sleep apnea occurs when your brain fails to send proper signals to the muscles in your body that control breathing. At this point, your body makes zero effort to breathe normally. Sufferers tend to wake feeling short of breath. They may also have a hard time falling and staying asleep. Central sleep apnea is also common in people with other underlying medical conditions including issues with brain functionality.
Complex Sleep Apnea Syndrome
This is the rarest form of sleep apnea and combines the effects of both obstructive and central sleep apnea. Generally, doctors will first treat obstructive sleep apnea using a CPAP (continuous positive airway pressure) machine (more on this later). If the problem persists, it’s assumed that central sleep apnea is also at play and alternative treatment options are explored.
Symptoms and Warning Signs of Sleep Apnea
With 70% of adults reporting at least one night of insufficient sleep a month, the signs of sleep apnea often go undetected as a case of transient insomnia. Left untreated, all forms of sleep apnea can wreak havoc on your health, which is why knowing and recognizing the warning signs and symptoms is crucial for finding the right treatment.

Symptoms include, but aren’t limited to:
- Gasping for air while sleeping
- Snoring
- Periods of stopped breathing during sleep (this is usually reported by another person i.e. a spouse, partner, or roommate)
- Daytime sleepiness
- Difficulty staying awake
- Dry mouth upon waking
- Waking with a headache
- Irritability due to lack of sleep
- Inability to focus during the day
Many of these symptoms are directly related to lack of sleep. Most sleep apnea sufferers don’t realize they’re not getting a restful night’s sleep. They think they’re sleeping fine when in actuality, your body is in a constant state of alertness and struggle. As your oxygen levels decrease, your heart rate spikes, putting strain on the cardiovascular system.
Health Complications Associated with Sleep Apnea
The inability to breathe naturally and consistently throughout the night can cause a long list of medical issues. It’s during sleep that your body recovers, repairs itself, and rejuvenates for the next day. Without adequate rest, your body and mind can’t function properly. Your body also goes through a lot of physical distress during these sleep apnea episodes.

Here are some of the most common and serious complications associated with sleep apnea.
High Blood Pressure and Cardiovascular Issues
During sleep apnea, your blood oxygen levels drop quickly and significantly. This can increase your blood pressure, putting extreme strain on your heart and entire cardiovascular system.
Patients with obstructive sleep apnea are most at risk for high blood pressure. These individuals are also in danger of heart attack, stroke, atrial fibrillation, and abnormal heartbeat. Patients with preexisting heart disease are at especially high risk. Repeated drops in blood oxygen levels can cause an irregular heartbeat, leading to death.
Type 2 Diabetes
Type 2 diabetes is caused by insulin resistance. Some studies show that sleep apnea increases your risk of developing insulin resistance, causing type 2 diabetes.
Metabolic Syndrome
A common link between metabolic syndrome and sleep apnea is obesity. Individuals with obesity are 77% more likely to develop sleep apnea. Metabolic syndrome is a combination of various health conditions including high blood pressure and sugar, abnormal cholesterol levels, and excess fat around the waist. People with this condition are at much greater risk of heart disease.
Liver Conditions
Sleep apnea sufferers are more likely to suffer from nonalcoholic fatty liver disease, which creates excess scarring on the organ. Many sleep apnea patients can also develop abnormal liver function.
Complications with Surgery or Medication Use
Obstructive sleep apnea can interfere with the effectiveness of certain medications, including general anesthesia. Due to your body’s inability to breathe normally, sleep apnea sufferers are at greater risk of complications following major surgery. Lying on your back and being sedated only add to these risks.
Risk Factors of Sleep Apnea
So, who exactly is at the greatest risk of developing sleep apnea? While patients range in age and gender, certain demographics and underlying medical conditions make you more susceptible to developing this specific sleep disorder.

Here are the key risk factors for both obstructive and central sleep apnea.
Medical History
Certain medical conditions put you at greater risk for developing obstructive sleep apnea. The irony here is that many of these conditions are also ones caused by sleep apnea. These include high blood pressure, type 2 diabetes, and congestive heart failure. In addition, those with Parkinson’s disease and chronic lung disease are also at increased risk. Women with Polycystic ovary syndrome and other hormonal disorders are more likely to fall victim to obstructive sleep apnea. Your family history may also act as a prelude to you developing sleep apnea later in life.
Men
Speaking of women, it’s actually more likely for men to develop this condition than their female counterparts. In fact, men are nearly 3 times more likely to have sleep apnea than women. A woman’s risk significantly rises after menopause and if you’re overweight. It’s important to note that the latter isn’t specific to women.
Obesity
As mentioned above, individuals who are significantly overweight are much more likely to develop obstructive sleep apnea. Extra fat deposits in your airways can easily obstruct your airways, interfering with regular breathing (and sleeping) rhythms. It’s also interesting to note that individuals with a greater neck circumference are more at risk due to narrowed airways. This can also be an inherited condition. Some people’s adenoids or tonsils are larger than others, causing an obstruction.
Alcohol and Nicotine Use
On their own, excessive alcohol intake and nicotine use are unhealthy habits that create countless health issues. When discussing these habits in relation to sleep apnea, they also put you at greater risk for a narrowed or obstructed airway. Smokers are 3 times more likely to have obstructive sleep apnea. Inflammation along with fluid retention in the throat and airways creates a blockage. When you drink alcohol, the muscles in your throat relax, even more, worsening the condition.
Prolonged opioid use can also lead to sleep apnea. Long-acting narcotics like methadone are the biggest culprit when discussing long-term sleep disorders.
Nasal Congestion
Sinus infections and common nasal congestion can also make breathing difficult and, eventually, lead to sleep apnea. Congestion caused by asthma or allergies makes it harder for you to breathe through your nose and for oxygen to freely move through your airways.

Aging
Unfortunately, wrinkles aren’t the only things older adults need to contend with. As your age increases, so does your risk of developing obstructive sleep apnea.
Stroke
Following a stroke, patients are between 50% to 70% more likely to develop obstructive sleep apnea. This risk decreases slightly to between 6% and 24% when discussing central sleep apnea. Sleep apnea can also increase your likelihood of having a stroke in the future by up to 3 times. The more severe your sleep disorder, the higher your risk of having a stroke.
Diagnosing Sleep Apnea
If you suspect you have sleep apnea, it’s best to seek an official medical diagnosis. Your doctor will evaluate your symptoms, medical history, and ask detailed questions about your sleep habits. They may also ask to speak with other members of your household who can offer an inside perspective on your sleep patterns.

At a sleep disorder center, a sleep specialist can help further evaluate your condition and make a final diagnosis. Some sleep centers require patients to stay the night for monitoring, while others will provide an at-home sleep study. For this, you’ll attach sensors to your body that will monitor your breathing and other bodily functions as you sleep. The equipment will monitor your blood oxygen levels, heart rate, lung, and brain activity. Using these results, doctors can determine the severity of your sleep apnea and offer treatment options.
Treatment Options for Sleep Apnea
Now that you have a better understanding of what causes sleep apnea and what exactly it is, let’s discuss treatment options.

Lifestyle Changes
For mild cases of sleep apnea, your doctor may recommend lifestyle changes. This includes losing excess weight, quitting smoking, or ceasing other unhealthy habits including alcohol and drug use. Sleep apnea caused by nasal congestion may be treated with allergy medication.
If your condition escalates from mild to severe, you may need to explore other treatment options.
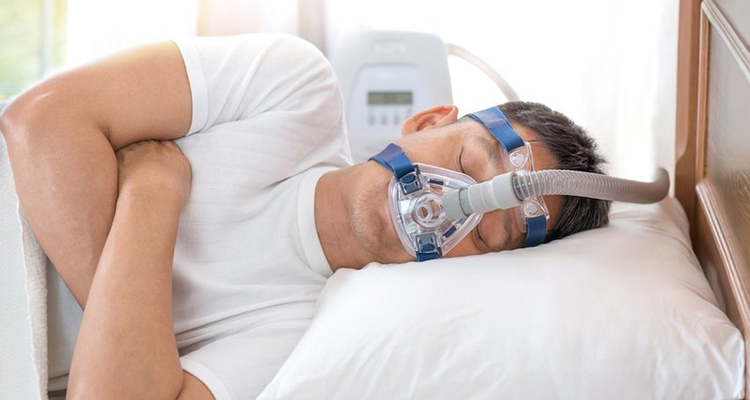
Continuous Positive Airway Pressure Machine (CPAP)
This is the most popular way to treat sleep apnea. With over 8 million CPAP users in the United States, this is one of the most popular and effective treatment options for sleep apnea. This machine delivers air pressure through a mask while you sleep to help keep your upper airway passages open. This prevents your throat from narrowing and you from having breaks in your breathing. It may also help reduce snoring.
The only downside to this treatment option is that wearing a CPAP mask isn’t always comfortable while sleeping. It will take time and practice to find a comfortable sleeping position while wearing a CPAP mask. For those that stick with it, the benefits far outweigh the discomfort.
Keep in mind that if you follow the doctor’s recommendation to lose weight, the level of air pressure on your CPAP may need adjusting.
Other Breathing Devices
Although the CPAP is the most common airway pressure device, there are other options out there. These include a BPAP (bilevel positive airway pressure) machine which provides more pressure with every inhale and less pressure as you exhale.
An adaptive servo-ventilation (ASV) is a relatively new airflow device that matches your normal breathing patterns, storing the information inside an internal computer. While sleeping, the machine works to normalize your breathing patterns and prevents you from taking pauses in your breathing.
Your doctor might also recommend an oral appliance that keeps your throat open during sleep, preventing any airway obstructions. These devices are often fitted by your dentist.
Surgery
In extreme cases of sleep apnea, a doctor might recommend surgery. This is the last resort option if all others fail. Surgical options include tissue shrinkage or removal, jaw repositioning, implants, nerve stimulation, and creating a new air passageway known as a tracheostomy.
Some recommended surgeries treat the cause, rather than the disorder itself. For example, weight-loss surgery or removing the tonsils or adenoids might help reduce the effects of sleep apnea.
The Difference Between Sleep Apnea and Insomnia
Sleep apnea is a common and serious sleep disorder that causes people to stop breathing during sleep. As your body struggles for air, you’re momentarily rustled awake. You may not realize you have sleep apnea at first. For some people, it takes months or even years of warning signs for them to take action. That, or another member of the household mentioning excessive snoring or gasping for air.

Insomnia, on the other hand, is the inability to fall asleep or stay asleep. Insomnia is caused by a long list of conditions, both medical and psychological. Stress, depression, and anxiety are all common causes of insomnia. Medical conditions like chronic pain, digestive issues, and Alzheimer’s disease can also lead to disturbances in sleep. Transient insomnia is caused by a specific event or trigger and generally dissipates after a few days.
The biggest difference between sleep apnea and insomnia is that sleep apnea is a medical condition that can cause serious health complications, including death. The inability to breathe properly during the night and dips in both blood pressure and oxygen levels can cause a disruption in sleep patterns, synonymous with insomnia. Insomnia, on the other hand, can cause sleep apnea.
These two conditions share many of the same signs and symptoms including:
- Daytime fatigue
- Inability to focus
- Irritability
- Trouble staying asleep
Even though some of the symptoms are the same, sleep apnea and insomnia are two very different conditions. Although chronic insomnia can cause health issues and complications, sleep apnea is a serious medical condition that needs immediate diagnosis.
Symptoms associated with sleep apnea and not with insomnia include:
- Snoring
- Headaches
- Dry mouth
- Drops in oxygen levels
- Difficulty breathing
A sleep specialist or doctor can help determine if you have sleep apnea or a certain type of insomnia. After reaching a diagnosis, you can explore different treatment options.
Treatment for Insomnia
It’s important to note that most cases of insomnia can be treated through behavioral therapy and lifestyle changes. Transient, or acute, insomnia usually dissipates on its own. If you’re faced with chronic insomnia or any type of insomnia not associated with a medical condition like sleep apnea, there are several treatment options available.

Cognitive Behavioral Therapy
Cognitive Behavioral Therapy (CBT) is a therapy treatment that addresses your anxieties over insomnia and then replaces these with healthier alternatives and benefits. Several different approaches fall under the umbrella of CBT for insomnia including stimulus control, sleep hygiene and education, relaxation methods, and sleep restriction or compression.
Lifestyle Changes
Similar to sleep apnea treatment, certain lifestyle changes can help ease the symptoms of insomnia. Avoiding heavy meals right before bed, adopting a healthy sleep routine, and reducing screen time are all effective methods. Meditation and mindfulness are also said to ease insomnia symptoms and help sufferers achieve better, deeper, and longer sleep.
Medication
Similar to surgery as the last resort for sleep apnea patients, medication can help those suffering from severe cases of insomnia. Some popular medications include BZD (Benzodiazepines), Nonbenzodiazepines (Z), and Orexins. For a more natural approach, try chamomile tea, melatonin, or essential oils for relaxation and calm.
Recognize the Warning Signs of Sleep Apnea vs. Insomnia
It’s important to understand the similarities and differences between these two sleep disorders. Insomnia, while serious, can be both acute and chronic. Sleep apnea can cause some dangerous side effects including heart attack, stroke, and death.

Whether you’re looking for relief from one or both of these conditions or simply want to achieve a more restful night’s sleep, Somnus can help. Using a combination of meditation, CBT, sleep restriction therapy, and stimulus control therapy, we help patients achieve the blissful night’s sleep they’ve always dreamed of. Our unique methods are designed to accommodate the needs and preferences of all users.
If you’re ready to embrace deep, blissful sleep, click here and get started today!

















